Advanced Technology Can Advance Functional Ability
It is common for health services to prescribe inexpensive devices with restricted function to limited community walkers.
Prosthetic interventions that are specifically designed for the biomechanical requirements of the older user could help reduce the risk of falls, maintain greater mobility and independence, improve quality of life and help reduce the long term burden on health care services.
Hydraulic Ankle Technology
Conventional prostheses are usually firmly attached to the shin or ‘pylon’ and rely on the deflection or deformation of polymeric foot components to replicate the dorsiflexion and plantarflexion behaviour of the natural ankle.
Models of the biological foot have shown that this elastic behaviour is present at normal walking speeds43. However, at slow speeds, the ankle becomes a net absorber of energy and the elastic model no longer fits43. The viscoelastic behaviour of hydraulic ankles better replicates natural ankle biomechanics.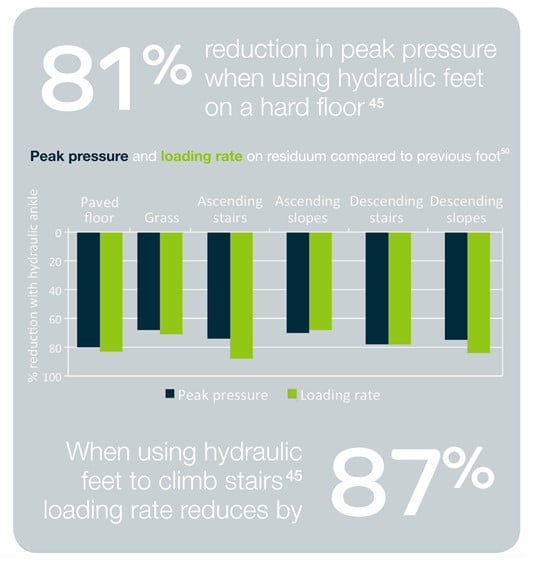
Hydraulic ankle technology has been proven to provide a number of benefits to elderly amputees. During walking, the deformable components of a prosthesis are deflected when loaded and return to their original position when unloaded.
With a hydraulic ankle, when unloaded, the ankle joint remains in a dorsiflexed position, meaning that the toe clearance during swing phase is increased by 18%44 so there is less chance of catching the foot on the ground or another object and a trip occurring.
The damped motion of the ankle joint also absorbs energy and reduces the loading on the residual limb within the socket. One study measured reductions in peak pressures by up to 81% and in the rate of loading by up to 87%, during a number of different everyday activities45.
Hydraulic prosthetic ankles seek to mimic biological ankle action with a hydraulically-damped, articulating joint in combination with the deformable foot.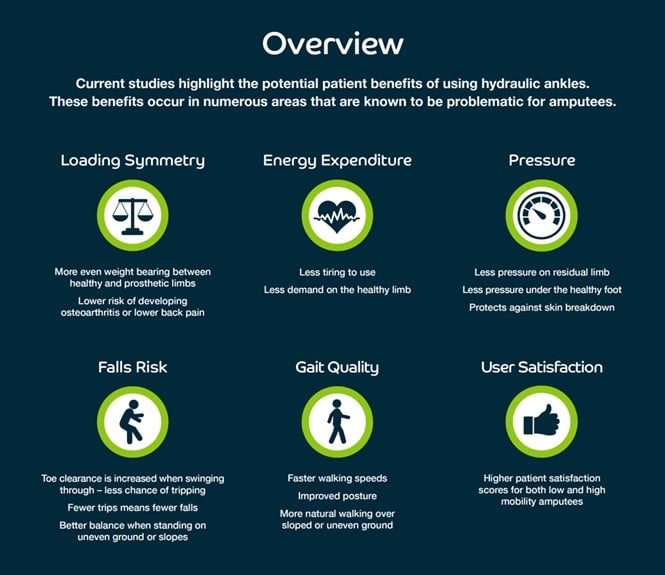
Biomimicry Allows for Safer Movement
Blatchford hydraulic ankles respond to the design specifications that natural movement dictates, fine-tuning joint position to align the body for optimum posture and comfort.
By continuously adjusting to absorb and release energy, our hydraulic ankles allow for an efficient roll-over, remaining perfectly aligned with the user for the next step to help reduce the risk of falls.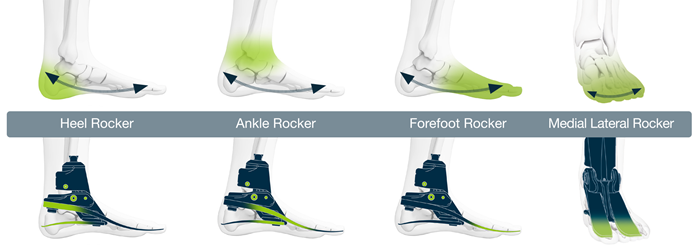
The best prosthesis replicates the dynamic and adaptive qualities of natural limb movement. This approach has resulted in the design of the world’s first hydraulic ankle-foot and award-winning technology by the Blatchford team.
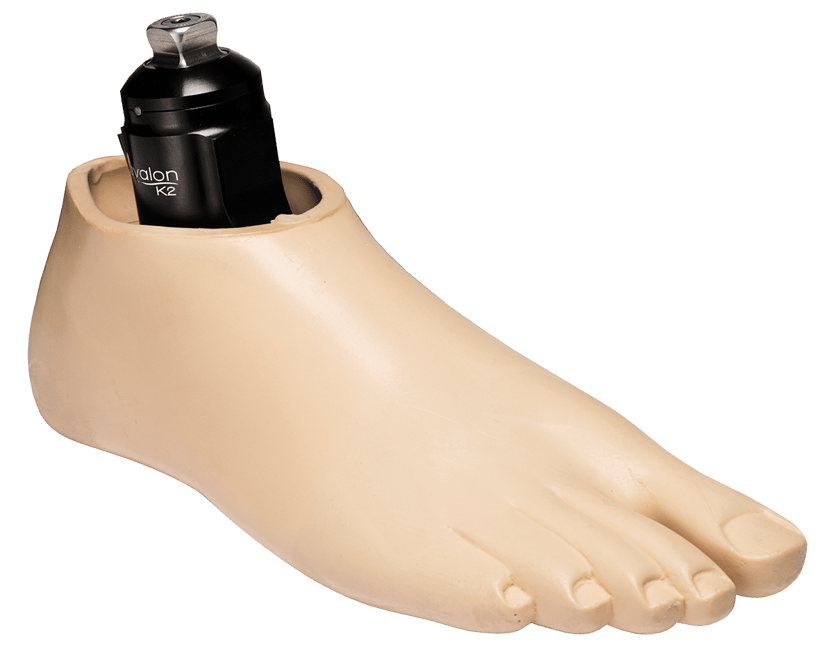
Avalon K2
AvalonK2 is our biomimetic hydraulic ankle that has been designed specifically for the complex needs of limited community ambulators. For K-2 level patients.
Avalon K2VAC
AvalonK2VAC combines the award winning AvalonK2 biomimetic hydraulic ankle with an integrated elevated vacuum system. This combination offers K2 users a unique product that both improves safety and long term health, and increases the feeling of socket security. For K-2 level patients.

Echelon
The award-winning Echelon is a waterproof hydraulic ankle that absorbs and damps on impact, self-aligns on rough and sloping surfaces, then remains dorsiflexed at toe-off. These design features help reduce abnormal pressures at the socket interface and other joints, promote comfort and postural symmetry to help reduce the risk of falls and preserve musculoskeletal health. For K-3 level patients. PDAC approved for the USA.

Echelon ER
Featuring an all-new robust and waterproof design, the extended range provides users with even more ground compliance on steep slopes and uneven terrain. Combined with improved accommodation of heel height, users have greater flexibility with footwear choice and a seamless transition to barefoot walking is possible.

Echelon VT
EchelonVT combines the advanced hydraulic technology of Echelon with an additional rotation and vertical shock absorption element, to reduce the shear forces at the socket interface. This means the user is able to move and adapt more freely, making EchelonVT ideal for taking part in activities such as golf and hiking.

Echelon VAC
By harnessing natural ankle motion, EchelonVAC quietly creates elevated vacuum, helping to maintain an optimally fitting socket throughout the day.

Elan
Elan is a microprocessor foot that mimics natural muscle resistance and ankle motion by adapting hydraulic resistance levels to optimise stability when standing and walking, on slopes and uneven terrain.

Elan IC
ElanIC is the world’s lightest and most compact waterproof microprocessor hydraulic ankle.

Hydraulic Ankles
Clinical Evidence
Over a decade after challenging conventional wisdom, new scientific evidence continues to be published on the medical advantages of hydraulic ankles.

Clinical Compendium
Blatchford Biomimetic Hydraulic Technology mimics the dynamic and adaptive qualities of muscle actuation to encourage more natural gait.
Multiple independent scientific studies, comparing Blatchford hydraulic ankle-feet to non-hydraulic feet, have shown:
- Greater comfort, reduced socket pressures
- Improved safety, reduced risk of trips and falls
- Smoother, easier and more natural gait
- More evenly balanced inter-limb loading
- Greater satisfaction

Introducing
Orion3
A microprocessor controlled hydraulic knee with intelligent speed control.
Features
• Situational Awareness – senses movement and speed to respond accordingly, in real time.
• Enhanced Stability Performance – 5 levels of stance resistance
- Controlled Stance Support
- Standing Support
- Dynamic Slope and Stair Descent
- Stumble Recovery
- Supported Sitting
• Natural Efficient Motion - MPC pneumatics ensure smooth swing at multiple speeds
- Optimal Stance Release
- Adaptive Speed Control
- Terminal Swing Damping
• Cycling Mode and Fixed Angle Flexion Lock Mode
• Knee Flexion to 130°
• Intuitive Programming Software via PC or App
• Lithium Ion batteries with up to 3 days life
• Battery Life Indicator and Low Power Mode
Hydraulic Ankle Technology
-
References
- Office for National Statistics (ONS). Population Estimates for UK, England and Wales, Scotland and Northern Ireland: mid-2016.2017.
- Aging Statistics [Internet]. [cited 2016 Sep 27]. Available from: http://www.aoa. acl.gov/Aging_Statistics/index.aspx
- Global ageing statistics | Data on ageing | HelpAge International [Internet]. [cited 2016 Sep 27]. Available from: http://www.helpage.org/resources/ageing-data/ global-ageing-statistics/
- Halter JB, Musi N, Horne FM, Crandall JP, Goldberg A, Harkless L, et al. Diabetes and cardiovascular disease in older adults: current status and future directions. Diabetes. 2014;63(8):2578–2589.
- Scottish Physiotherapy Amputee Research Group (SPARG). A Survey of the Lower Limb Amputee Population in Scotland. 2010.
- Fletcher DD, Andrews KL, Butters MA, Jacobsen SJ, Rowland CM, Hallett JW. Rehabilitation of the geriatric vascular amputee patient: a population-based study. Arch Phys Med Rehabil. 2001;82(6):776–779.
- Ziegler-Graham K, MacKenzie EJ, Ephraim PL, Travison TG, Brookmeyer R. Estimating the prevalence of limb loss in the United States: 2005 to 2050. Arch Phys Med Rehabil. 2008;89(3):422–429.
- Prince F, Corriveau H, Hébert R, Winter DA. Gait in the elderly. Gait Posture. 1997;5(2):128–135.
- Hageman PA, Blanke DJ. Comparison of gait of young women and elderly women. Phys Ther. 1986;66(9):1382–1387.
- Kerrigan DC, Lee LW, Collins JJ, Riley PO, Lipsitz LA. Reduced hip extension during walking: healthy elderly and fallers versus young adults. Arch Phys Med Rehabil. 2001;82(1):26–30.
- Judge JO, Davis RB, Õunpuu S. Step length reductions in advanced age: the role of ankle and hip kinetics. J Gerontol A Biol Sci Med Sci. 1996;51(6):M303– M312.
- Kerrigan DC, Todd MK, Della Croce U, Lipsitz LA, Collins JJ. Biomechanical gait alterations independent of speed in the healthy elderly: evidence for specific limiting impairments. Arch Phys Med Rehabil. 1998;79(3):317–322.
- Kerrigan DC, Lee LW, Nieto TJ, Markman JD, Collins JJ, Riley PO. Kinetic alterations independent of walking speed in elderly fallers. Arch Phys Med Rehabil. 2000;81(6):730–735.
- Owings TM, Grabiner MD. Variability of step kinematics in young and older adults. Gait Posture. 2004;20(1):26–29.
- Brach JS, Studenski S, Perera S, VanSwearingen JM, Newman AB. Stance time and step width variability have unique contributing impairments in older persons. Gait Posture. 2008;27(3):431–439.
- Mills PM, Barrett RS. Swing phase mechanics of healthy young and elderly men. Hum Mov Sci. 2001;20(4):427–446.
- Riley PO, Schenkman ML, Mann RW, Hodge WA. Mechanics of a constrained chair-rise. J Biomech. 1991;24(1):77–85.
- Papa E, Cappozzo A. Sit-to-stand motor strategies investigated in able-bodied young and elderly subjects. J Biomech. 2000;33(9):1113–1122.
- Shepherd RB, Koh HP. Some biomechanical consequences of varying foot placement in sit-to-stand in young women. Scand J Rehabil Med. 1996;28(2):79–88.
- Janssen WG, Bussmann HB, Stam HJ. Determinants of the sit-to-stand movement: a review. Phys Ther. 2002;82(9):866–879.
- Bernardi M, Rosponi A, Castellano V, Rodio A, Traballesi M, Delussu AS, et al. Determinants of sit-to-stand capability in the motor impaired elderly. J Electromyogr Kinesiol. 2004;14(3):401–410.
- Kawagoe S, Tajima N, Chosa E. Biomechanical analysis of effects of foot placement with varying chair height on the motion of standing up. J Orthop Sci Off J Jpn Orthop Assoc. 2000;5(2):124–33.
- WISQARS (Web-based Injury Statistics Query and Reporting System)|Injury Center|CDC [Internet]. [cited 2016 Aug 18]. Available from: https://www.cdc.gov/ injury/wisqars/
- Miller WC, Speechley M, Deathe B. The prevalence and risk factors of falling and fear of falling among lower extremity amputees. Arch Phys Med Rehabil. 2001;82(8):1031–1037.
- Hausdorff JM, Edelberg HK, Mitchell SL, Goldberger AL, Wei JY. Increased gait unsteadiness in community-dwelling elderly fallers. Arch Phys Med Rehabil. 1997;78(3):278–283.
- Hausdorff JM, Rios DA, Edelberg HK. Gait variability and fall risk in communityliving older adults: a 1-year prospective study. Arch Phys Med Rehabil. 2001;82(8):1050–1056.
- Barak Y, Wagenaar RC, Holt KG. Gait characteristics of elderly people with a history of falls: a dynamic approach. Phys Ther. 2006;86(11):1501–1510.
- Barrett RS, Mills PM, Begg RK. A systematic review of the effect of ageing and falls history on minimum foot clearance characteristics during level walking. Gait Posture. 2010;32(4):429–435.
- Tromp AM, Pluijm SMF, Smit JH, Deeg DJH, Bouter LM, Lips P. Fall-risk screening test: a prospective study on predictors for falls in community-dwelling elderly. J Clin Epidemiol. 2001;54(8):837–844.
- Important Facts about Falls | Home and Recreational Safety | CDC Injury Center [Internet]. [cited 2016 Aug 18]. Available from: http://www.cdc.gov/ homeandrecreationalsafety/falls/adultfalls.html
- Hunter SW, Batchelor F, Hill KD, Hill A-M, Mackintosh S, Payne M. Risk factors for falls in people with a lower limb amputation: a systematic review. PM&R. 2016
- Kulkarni J, Wright S, Toole C, Morris J, Hirons R. Falls in patients with lower limb amputations: prevalence and contributing factors. Physiotherapy. 1996;82(2):130–136.
- Alexander BH, Rivara FP, Wolf ME. The cost and frequency of hospitalization for fall-related injuries in older adults. Am J Public Health. 1992;82(7):1020–1023.
- Sterling DA, O’Connor JA, Bonadies J. Geriatric falls: injury severity is high and disproportionate to mechanism. J Trauma Acute Care Surg. 2001;50(1):116–119.
- Miller WC, Deathe AB. The influence of balance confidence on social activity after discharge from prosthetic rehabilitation for first lower limb amputation. Prosthet Orthot Int. 2011;35(4):379–385.
- Costs of Falls Among Older Adults | Home and Recreational Safety | CDC Injury Center [Internet]. [cited 2016 Aug 18]. Available from: http://www.cdc.gov/ homeandrecreationalsafety/falls/fallcost.html
- Stevens JA, Corso PS, Finkelstein EA, Miller TR. The costs of fatal and non-fatal falls among older adults. Inj Prev. 2006;12(5):290–295.
- Burke MJ, Roman V, Wright V. Bone and joint changes in lower limb amputees. Ann Rheum Dis. 1978;37(3):252–254.
- Kulkarni J, Adams J, Thomas E, Silman A. Association between amputation, arthritis and osteopenia in British male war veterans with major lower limb amputations. Clin Rehabil. 1998;12(4):348–353.
- Norvell DC, Czerniecki JM, Reiber GE, Maynard C, Pecoraro JA, Weiss NS. The prevalence of knee pain and symptomatic knee osteoarthritis among veteran traumatic amputees and nonamputees. Arch Phys Med Rehabil. 2005;86(3):487–493.
- Ehde DM, Czerniecki JM, Smith DG, Campbell KM, Edwards WT, Jensen MP, et al. Chronic phantom sensations, phantom pain, residual limb pain, and other regional pain after lower limb amputation. Arch Phys Med Rehabil. 2000;81(8):1039–1044.
- Kulkarni J, Gaine WJ, Buckley JG, Rankine JJ, Adams J. Chronic low back pain in traumatic lower limb amputees. Clin Rehabil. 2005;19(1):81–86.
- Hansen AH, Childress DS, Miff SC, Gard SA, Mesplay KP. The human ankle during walking: implications for design of biomimetic ankle prostheses. J Biomech. 2004;37(10):1467–1474.
- Johnson L, De Asha AR, Munjal R, Kulkarni J, Buckley JG. Toe clearance when walking in people with unilateral transtibial amputation: effects of passive hydraulic ankle. J Rehabil Res Dev. 2014;51(3):429.
- Portnoy S, Kristal A, Gefen A, Siev-Ner I. Outdoor dynamic subject-specific evaluation of internal stresses in the residual limb: hydraulic energy-stored prosthetic foot compared to conventional energy-stored prosthetic feet. Gait Posture. 2012;35(1):121–125.
- Adamczyk PG, Collins SH, Kuo AD. The advantages of a rolling foot in human walking. J Exp Biol. 2006;209(20):3953–3963.
- Hansen AH, Wang CC. Effective rocker shapes used by able-bodied persons for walking and fore-aft swaying: Implications for design of ankle–foot prostheses. Gait Posture. 2010;32(2):181–184.
- Hansen AH, Childress DS. Investigations of roll-over shape: Implications for design, alignment, and evaluation of ankle-foot prostheses and orthoses. Disabil Rehabil. 2010;32(26):2201–2209.
- Curtze C, Hof AL, van Keeken HG, Halbertsma JP, Postema K, Otten B. Comparative roll-over analysis of prosthetic feet. J Biomech. 2009;42(11):1746– 1753.
- Moore R. Effect on Stance Phase Timing Asymmetry in Individuals with Amputation Using Hydraulic Ankle Units. JPO J Prosthet Orthot. 2016;28(1):44– 48.
- Moore R. Patient evaluation of a novel prosthetic foot with hydraulic ankle aimed at persons with amputation with lower activity levels. JPO: Journal of Prosthetics and Orthotics. 2017;29(1):44-7.
- Sedki I, Moore R. Patient evaluation of the Echelon foot using the Seattle Prosthesis Evaluation Questionnaire. Prosthet Orthot Int. 2013;37(3):250–254.
- Barnett CT, Brown OH, Bisele M, Brown MJ, De Asha AR, Strutzenberger G. Individuals with Unilateral Transtibial Amputation and Lower Activity Levels Walk More Quickly when Using a Hydraulically Articulating Versus Rigidly Attached Prosthetic Ankle-Foot Device. JPO: Journal of Prosthetics and Orthotics. 2018;30(3):158-64.
